The global vitamin B12 supplement market is poised for significant growth in the upcoming years. Although daily oral vitamin B12 supplements typically contain doses far exceeding the recommended amount, the impact of such high levels of vitamin B12 on gut health remains unclear.
In a recent paper, Samantha Gruenheid, Chair of the Department of Microbiology and Immunology at McGill, and a team of scientists from across Canada unraveled the fascinating connections between vitamin B12 and the gut microbiome, illuminating the potential health consequences of over-supplementation. Over-supplementation, they proved, can perturb gut health.
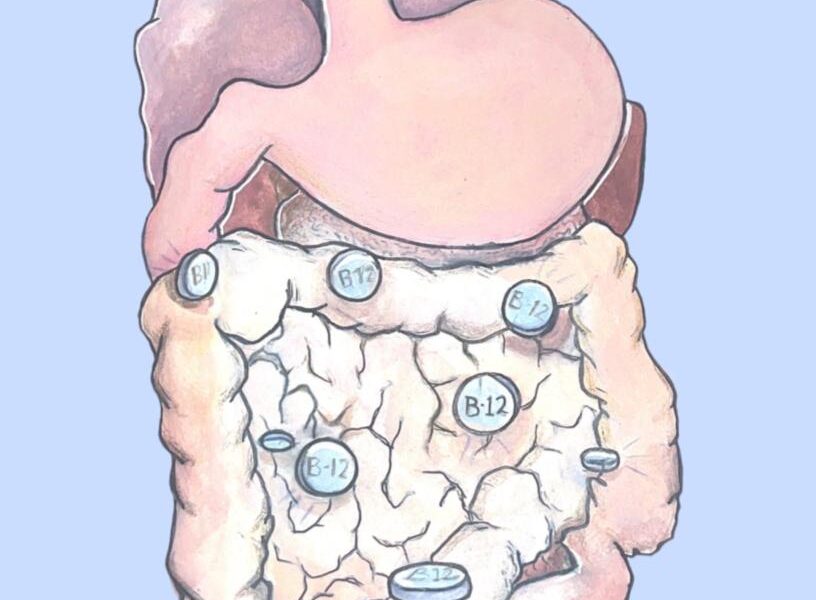
Vitamin B12, also known as cobalamin, is crucial to the function of nerve cells and the formation of red blood cells and DNA. We most often consume it via supplements, animal food products, fortified plant-based foods, and fermented foods.
In the digestive system, the small intestine absorbs most of the B12 that you eat. The liver stores any excess after it has been excreted via bile. The remaining B12, unabsorbed by the liver, then enters the gut microbiota—a system of microorganisms, including bacteria, fungi, and viruses, in one’s gastrointestinal system.
The recommended daily vitamin B12 intake for those ages 14 and older is 2.4 micrograms. Although a high vitamin B12 intake is generally considered safe, Gruenheid’s findings suggest that it may disrupt the gut microbiota’s activities.
The researchers evaluated the effect of vitamin B12 on the gut microbiota of mice by providing a vitamin B12 supplementation proportionate to 25 milligrams in humans.
“The reason we selected this amount was based on a mislabelled commercially available mouse diet,” Gruenheid said in an interview with The Tribune. “Fortunately, the dose was also a good estimation of the dose in some human supplements. Some supplements are approximately 1000 times the recommended daily intake, which is approximately what we achieved in this study.”
The researchers found that vitamin B12 supplementation increased susceptibility to infection with Citrobacter rodentium—a mouse-specific pathogen.
“There are two things that are contributing to this. One factor is this inflammatory environment created by vitamin B12 over-supplementation,” Ben Willing, associate professor in the Department of Agricultural, Food, and Nutritional Science at the University of Alberta, said in an interview with The Tribune. “Another factor is the Citrobacter bacteria itself, which competes for vitamin B12. With large amounts of vitamin B12 available in the gut, it is easier for Citrobacter bacteria to get vitamin B12, meaning that they are better able to colonize and induce an infection.”
Increased levels of inflammatory biomarkers, such as interleukin-12 and interleukin-17, indicate the inflammation caused by vitamin B12 over-supplementation.
“We believe that, even in the absence of the pathogen, vitamin B12 over-supplementation disrupts the ecosystem of the microbes because we have changed one of the things that microbes compete for and share,” Willing said.
In other words, excessive amounts of vitamin B12 can disrupt the microbial community in the gut.
“There is a potential for vitamin B12 supplements to change and even disrupt the competition dynamics in the gut microbiome,” Willing said. “On a larger scale, this study shows us an example of a health consequence when we add something to the diet.”
Vitamin B12 does play an essential role in ensuring health, and it may be a good idea for older individuals and those who do not eat animal products to take a vitamin B12 supplement of approximately 2.4 micrograms to ward off vitamin B12 deficiency. However, as Gruenheid’s study has demonstrated, it is crucial to pay more attention to the amount of vitamin B12 in each supplement since an extremely high dose of vitamin B12 can engender unintended health consequences.