Alzheimer’s disease (AD) is a progressive neurodegenerative disease that affects memory, thinking, and eventually grows severe enough to interfere with daily life. AD is the most common cause of dementia, an umbrella term that encompasses many different symptoms of cognitive decline.
While AD is still categorized as an incurable disease, researchers continue to look for treatments to improve the lives of patients and their families. With promising developments emerging in the field, could AD research be entering a new era? Experts such as Dr. Serge Gauthier, a professor of McGill’s Department of Neurology and Neurosurgery and Department of Psychiatry, suggest that it may be.
As director of the Alzheimer’s Disease and Related Disorders Research Unit at the Douglas Research Centre, Gauthier’s research aims to expand treatment options and advance earlier intervention for patients. Like many clinicians, Gauthier’s interest in pursuing AD research stemmed from a surprising encounter in the clinic.
“I met a 30-year-old woman with AD who came into our clinic,” Gauthier said in an interview with //The Tribune//. “It was a chance encounter, to meet someone so young with the disease, and it completely shocked me.”
There is a common misconception that AD can only develop in older adults, but Gauthier explained why this is not the case.
“Now, it’s well known that you can have three specific inherited [AD] genes, which can make symptoms emerge around age 30 to 40,” Gauthier said. “Over the years, we have developed a special network to treat people as young as 20 from those families.”
Gauthier then highlighted some of the biggest changes in AD research over the course of his career.
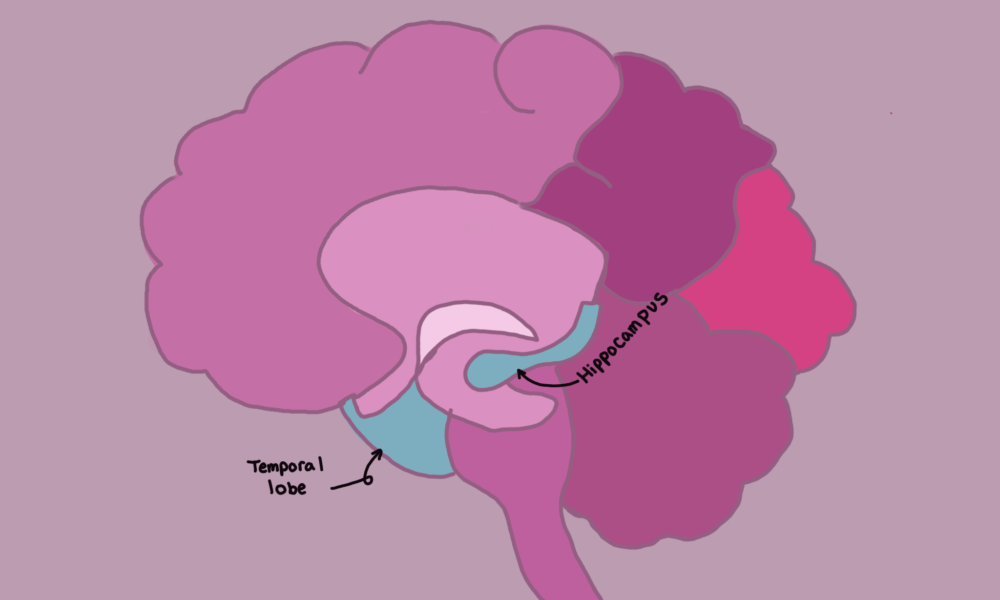
“The biggest change has been the definition of AD, which is now based on the presence of specific proteins in the brain, amyloid and tau. Strokes also play a big role, and there are other protein changes that come into play,” Gauthier said. “So AD is more complex [than previously thought], and we now may be able to say what kind of AD it is, what protein is most important for [a given patient’s AD], and [how to tailor] treatments to the patient’s [unique form of AD].”
AD is commonly thought to be just a normal part of aging, but Gauthier clarified the nuances here.
“Over age 70, everybody has slight short-term memory [decline], but as long as it does not interfere significantly with your daily life, it’s considered normal,” Gauthier said. “If you have hesitations for words or remembering appointments and it’s [affecting] your daily routine, you should see a clinician to see if it’s caused by medications, lack of thyroid hormone, poor sleep, or AD.”
Next, Gauthier explained the grey zone of AD—the ambiguous, early stage of the disease where mild symptoms begin to develop. At this stage, biomarkers such as amyloid accumulations can be seen on a PET scan.
“There is this grey zone that may last three to five years, where we see mild cognitive impairments, which are mostly memory-related. This zone is of interest because if it is caused by AD, we do have medications that could prolong this more benign stage and delay dementia.”
Vascular factors, such as diabetes, may also contribute to the development of AD, where damage to blood vessels may disrupt blood flow to the brain, resulting in damaged tissue.
Gauthier also discussed how socioeconomic factors play a role in the development of AD, where certain populations are at higher risk. He highlights the fourteen modifiable risk factors for dementia to be used as a helpful tool for the prevention of AD.
“Those less educated, with high blood pressure, and living in relative social isolation [are at highest risk],” Gauthier said. “It’s rarely one factor that you should pay attention to and more of a combination.”
Gauthier points to the Dementia Education Program as a helpful resource for the patients’ loved ones who are undeniably impacted by AD’s effects.
“The dementia education program is focused on caregiver needs and resources […] helping educate people and give them a place where they can talk about what they’re living through.”As the population of older adults continues to rise, so does the urgency of addressing AD and its wide-reaching effects on patients, caregivers, and healthcare systems. With over 40 years of experience, Gauthier remains optimistic about the direction AD research is heading. With blood tests, clinical trials, and FDA-approved medications on the way, the field is moving toward earlier diagnosis and more individualized treatment options.